Five Things To Consider if You Have Chronic Bladder Pain With Endo
For many of us with endo, if we get pain in the bladder or urethra or have problems urinating, we naturally might assume that endometriosis is on our bladder. While this can certainly be the case, it’s not always.
Of course, we want to rule this out as being a real possibility, so it’s important to work with a specialist endometriosis surgeon and team that can correctly identify endo on the bladder.
Exploring alternative causes of bladder and urethral pain in endometriosis
If you do get the all-clear, then here are five things to consider that may be contributing to your symptoms (and often are, even if endo is present in the bladder too):
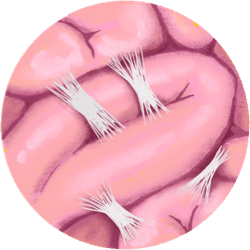
Adhesions
Adhesions are web-like structures of collagen that grow in response to a wound, injury, or infection. They are essentially scar tissue that works to protect and heal an area, but sometimes they are a little excessive and go too far. They can end up sticking to organs, wrapping round organs, and sticking organs together.
Adhesions put a huge amount of pressure on the organs they attach to, and this can cause significant pain and dysfunction, including bladder pain, trouble emptying your bladder, increased frequency, etc.
Adhesions don’t just grow as a result of endo itself but also following abdominal surgery. So, even if you’ve had all of your endo excised, that doesn’t mean you don’t have adhesions.
I recommend finding a specialist, such as a Clear Passage therapist or a Visceral Manipulation therapist, who can identify these adhesions and loosen/break them down.

Pelvic floor dysfunction
The pelvic floor is like a hammock of muscle and nerves holding your bladder, vagina, and bowel in place. These muscles and nerves control the function of these organs. So, if there’s a problem with the pelvic floor, you’ll likely going to feel it in one or all of these organs.
People with endometriosis tend to have what’s known as a tight pelvic floor after years of being in pain. This can result in bladder pain, urethra pain, problems urinating, and so on.
Working with a pelvic floor physiotherapist can help relieve pain and restore bladder function.

Inflammation
Some of us may have sensitivities to certain foods or compounds found in foods, like histamine. These irritants can actually bother the bladder lining and cause inflammation. Working with a specialist to identify your triggers and calm down the bladder can significantly help and, over time, you should be able to add some or most of these foods back in again.
Another factor to consider is that the presence of endometriosis in the pelvic cavity causes local inflammation. As a result, even if there aren’t endo lesions on or near the bladder, the nearby inflammation can actually begin to spread to the bladder and cause pain.
Calming down your body’s overall inflammatory response and perhaps taking targeted supplements for bladder inflammation can go a long way to alleviating pain.

Embedded UTI and biofilms
For some of us, our issues may be from chronic embedded urinary tract infections. UTIs can hide in a protective layer known as a biofilm and even embed themselves into the bladder wall, which makes testing for them much harder. Working with a practitioner who can order you more advanced testing (and may even use an antibiofilm to reveal hidden bacteria) can help you discover the source of your pain.1,2
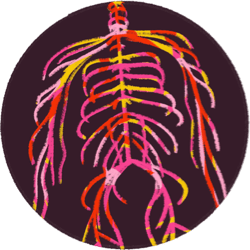
Nervous System Dysregulation
Your nervous system is, in short, responsible for how loud or quiet pain is. After years of chronic stress and pain from living with endo, you may find your pain volume is stuck on "loud." This doesn’t mean your pain isn’t real. It absolutely is, but all pain is the result of nerves and the brain working together to decide whether to produce pain and how severe it should be.3
The good news is that we can calm the nervous system down and teach the brain to feel safer in our body, and this can significantly reduce that volume. Have a listen to this podcast episode to understand how.
Join the conversation