Looking at Cystic Ovarian Endometriosis: What are Endometriomas?
Endometriosis is a significant reproductive health condition that can cause a variety of symptoms and complications, including pain and infertility. Getting an early and accurate diagnosis of endometriosis can help minimize and treat symptoms, as well as improve quality of life. There are different types of endometriosis, and knowing more about them can help you identify symptoms and make informed treatment decisions.
What is cystic ovarian endometriosis?
Cystic ovarian endometriosis is a type of endometriosis that is associated with ovarian and tubal adhesions, or scar-like tissue.1 These adhesions can cause infertility. This type of endometriosis is also associated with superficial pelvic endometriosis and deep endometriosis, as well as pelvic pain. Cystic ovarian endo affects 17-44 percent of women with endometriosis.2
What are endometriomas?
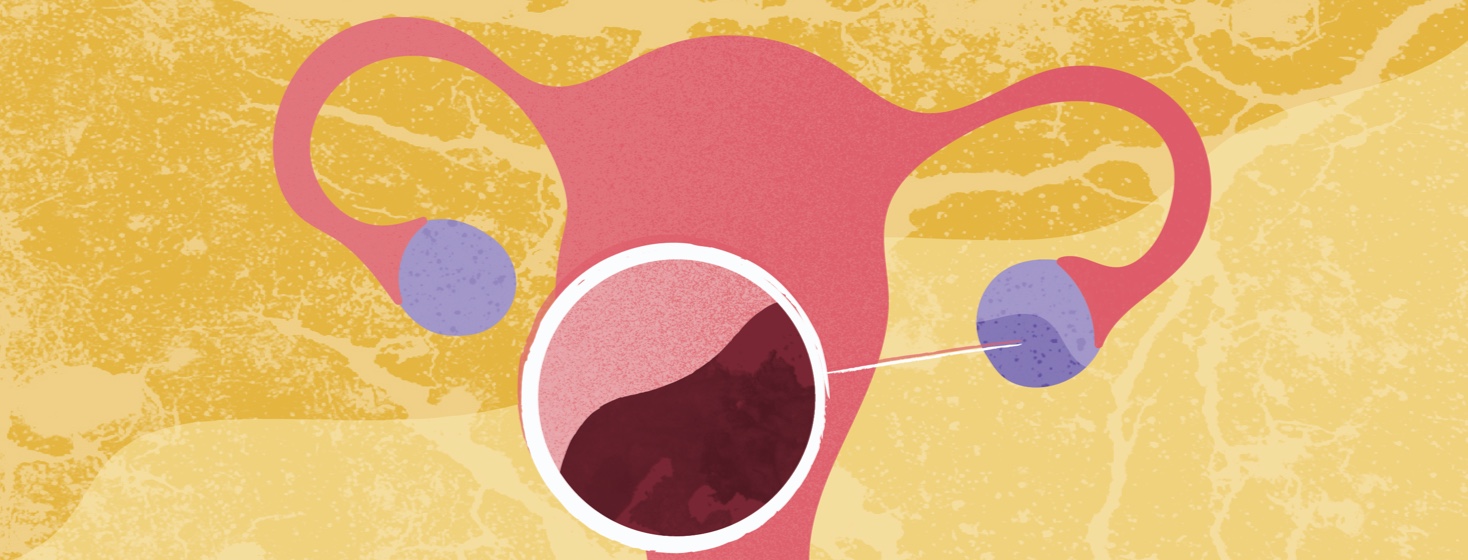
Although endometriosis is often found on the surface of the ovaries, it can also be found deep in the pelvis. 3 Cystic ovarian endometriosis creates dark cavities filled with thick, old blood called endometriomas or “chocolate cysts".2,3
According to our 2020 Endometriosis In America survey survey takers, 56 percent of endo warriors have been diagnosed with endometriomas.
Diagnosis is typically suspected upon seeing the images on an ultrasound of the pelvis, but can only be definitively diagnosed based on microscopic examination of the cyst.3 A transvaginal ultrasound can help differentiate an endometrioma from other benign ovarian tumors, but the gold standard for diagnosing endometriomas is laparoscopy.2
Endometriomas are very serious and have been associated with a variety of complications and health issues, including:3
- Higher risk of ovarian cancer in women of reproductive age
- Pelvic pain
- Infertility
- Decreased ovarian function
Endometriomas can also interfere with the efficacy of assisted reproductive technologies (ART). They can also destroy healthy ovarian tissue, leading to early ovarian failure or problems with ovarian function.
How are endometriomas treated?
Different health care providers have different opinions on the best way to treat endometriomas, but it is generally agreed upon that women with endometriomas who are of reproductive age should be treated by fertility specialists. Treatment options can include:3
- Observation of symptoms
- Observation via ultrasounds
- Medical treatment
- Surgical treatment
While observation and medical management of endometriomas are certainly options, they often do not treat the symptoms associated with endometriomas.3 If severe and chronic pelvic pain is an issue, surgery is typically recommended as a first-line treatment. Surgery is the main treatment for endometriomas, but this also depends on whether an individual is going to be having ART or not, as well as specific situations.
Conservative surgery that removes the endometriomas can be effective in not only relieving symptoms but it can also be fertility-enhancing. More than half of women in one major study who had infertility with no other cause became pregnant within 2 years of the endometrioma-removing surgery.3
For those women who are undergoing ART or planning to do ART, surgery is generally not recommended because it otherwise has no effect on pregnancy rates with ART, and it might actually reduce ovarian output of eggs. There are several situations where it is recommended, even in those doing ART, including:3
- The endometrioma significantly impairs egg retrieval
- The endometrioma is ruptured or infected at the time of egg retrieval
- The amount of ovarian stimulation necessary for ART is severely painful
- The endometrioma looks suspicious on radiologic imaging (for malignancy)
Surgical treatment success can vary, depending on the technique used and when it is done. Even minimally invasive and conservative surgery can cause permanent damage to the ovary.3 It is crucial to discuss all of the options with your specialist and treatment team, and make a decision with which you are comfortable, knowing the possible risks and benefits.
Join the conversation