What Is Endometriosis?
Reviewed by: HU Medical Review Board | Last reviewed: June 2018 | Last updated: December 2024
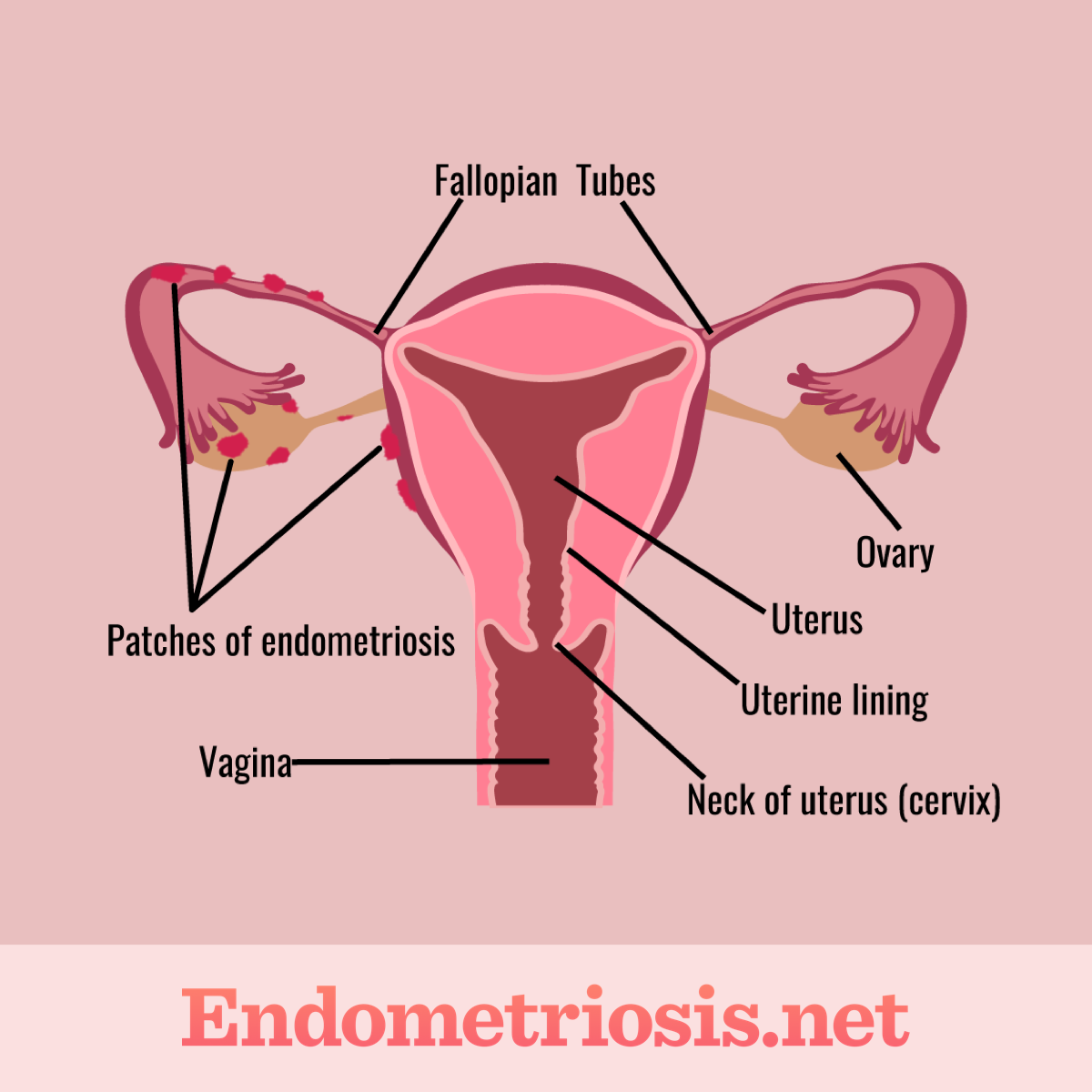
The tissue that lines the uterus is known as endometrium. This lining thickens each month during the menstrual cycle, and is shed as it breaks downs and bleeds during a woman’s period each month. Endometriosis is a chronic condition in which endometrial-like tissue grows outside of the uterus. For those with endometriosis, this tissue forms and grows in other places of the body. Most commonly, this abnormal tissue growth occurs in the fallopian tubes, ovaries, outer surface of the uterus, and other parts of the pelvis. Very rarely, endometriosis can affect other parts of the body including the lungs, skin, or brain. The displaced endometrial tissue still thickens and breaks down each month, however, there is no place for the blood to escape the body. This can lead to ovarian cysts, scar tissue, inflammation, pain, blockage of the fallopian tubes, and adhesions (fibrous tissues that can form between organs and connect them), among other issues.1-3
Figure 1. Female reproductive system
Endometriosis is often referred to as “endo” and the growths it causes are generally benign (non-cancerous or life-threatening). It has been estimated that endometriosis affects at least 11% of women in the United States, however, this number may underestimate the true proportion of women affected, as many do not show obvious symptoms of the condition and may not get properly diagnosed.1,2,4
Types of endometriosis
There are a variety of ways endometriosis can present for those who have the condition. Some of these different forms of endometriosis include:
- Superficial peritoneal endometriosis: Thin lesions form on the lining of the peritoneum (the lining that surrounds the pelvic cavity and some of the organs and structures within the pelvis)
- Ovarian endometriomas: Endometrial tissue and old blood collects in the ovaries as a result of endometriosis, leading to blood-filled cysts (also called chocolate cysts due to the color of the old blood). These cysts can grow and interfere with fertility, as well as potentially increase the risk of developing ovarian cancer
- Deep infiltrating endometriosis: Characterized by endometriosis lesions that have invaded the peritoneum five or more millimeters beyond the surface, into the retroperitoneal space further into the abdomen
- Endometriotic nodules: Hard masses composed of various tissue types (including endometrial, fat, and fibrous muscular tissue) that are most often found between the rectum and vagina. These nodules are often considered a form of deep infiltrating endometriosis, but their exact classification is currently up for debate1,5,6
Symptoms
Endometriosis can affect every individual differently. Some individuals experience extreme, debilitating, and life-changing symptoms, while others may be asymptomatic (experience no symptoms at all). It’s important to note, however, that the presence or level of severity of symptoms is not indicative of how far progressed or how serious an individual’s endometriosis is. For example, an individual in extreme pain may still have endometriosis that has not progressed as much as another individual who has no pain at all. Despite these differences, common symptoms of endometriosis include the following:
- Painful menstrual cramps or pelvic pain (also called dysmenorrhea)
- Pain during intercourse (also called dyspareunia)
- Infertility or difficulty becoming pregnant
- Excessive bleeding during periods or bleeding in between periods
- Intestinal discomfort or pain when going to the bathroom
- Digestive issues including constipation, bloating, diarrhea, and nausea
- Fatigue2,3
Causes
The exact cause of endometriosis is not known, however, the most common potential explanations include:
- Retrograde menstrual flow: Menstrual blood with endometrial cells and tissue can travel backwards through the fallopian tubes rather than out of the body. When this happens, these cells and tissue may stick to other parts of the body where they can continue to thicken and then breakdown
- Genetic factors: Often an individual with endometriosis also has a family member, or multiple family members, who have the condition as well
- Hormonal or immune response-related cell transformations: Some theories suggest that hormones or other immune system-related factors may be able to induce or influence other cells to behave like endometrial cells in other parts of the body
- Transport of endometrial cells: Endometrial cells may be able to travel to other parts of the body via the lymphatic system and blood vessels
- Surgical transport: Endometrial cells may be transported to other parts of the body or to surgical incision sites after a C-section, hysterectomy, or other abdominal or pelvic surgical procedure
- Other immune system-related dysfunction: It has been theorized that the immune system may fail to attack or remove endometrial cells if they do ever become misplaced2,3
Diagnosis
After recording your personal medical history and any symptoms you may be having, your doctor may recommend a pelvic exam or imaging tests such as an ultrasound or MRI (magnetic resonance imaging). These tests may help look for ovarian cysts which could point toward endometriosis. Additionally, they may prescribe medications such as hormonal birth control or medications called GnRH (gonadotropin-releasing hormone) agonists, which are both common endometriosis treatment options, to see if your symptoms respond.
Ultimately, the only way to receive a definitive diagnosis of endometriosis is with surgery. A minimally invasive surgery called a laparoscopy uses a small camera-containing tool to investigate the tissue in the uterus, pelvis, and other surrounding structures more carefully. Endometriosis lesions may be immediately visible inside the body in some cases, but in others, it may be necessary to take a small tissue sample and look at it under a microscope to accurately diagnose the condition.1-3
Treatment
There are several treatment options available for individuals with endometriosis. These include, but are not limited to:
- Hormonal therapy including contraceptives, GnRH agonists and danazol
- Surgery to remove endometriosis lesions or to remove the uterus and cervix (total hysterectomy)
- Pain medications including over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs)
For individuals looking to become pregnant, assisted reproductive technologies including in vitro fertilization, intrauterine insemination, and other methods may be used to increase the chance of pregnancy.1-3
Possible complications of endometriosis
Endometriosis has often been associated with an increased risk of having other health conditions, including, but not limited to:
- Pregnancy complications and infertility
- Autoimmune conditions
- Allergies or asthma
- Fibromyalgia
- Chronic fatigue syndrome
- Certain cancers, including ovarian cancer
- Depression and anxiety2
If you are concerned about your risk of developing or already having one or more of the above conditions, talk to your healthcare provider for more information on your specific situation.